Breast surgery refers to a group of procedures that alter the size, shape, position, or symmetry of the breasts. Although often associated with cosmetic change, breast surgery can also address physical discomfort, structural concerns, and the long-term effects of pregnancy, weight fluctuation, ageing, or previous operations.
Because the term covers several distinct procedures, understanding the differences between them is essential. Breast augmentation is not the same as a breast lift. A reduction addresses different concerns than fat transfer. Revision surgery has its own planning considerations. Clear definitions help patients move from vague goals to realistic expectations.
This guide explains the main types of breast surgery, how surgical planning works, what recovery involves, and the long-term factors that should be considered before making a decision.
What Is Included Under Breast Surgery?
Breast surgery is an umbrella term rather than a single operation. It includes procedures designed to increase volume, reduce size, reposition tissue, improve contour, or correct previous surgical outcomes.
The most common types of breast surgery include breast augmentation, breast lift (mastopexy), breast reduction, implant removal or exchange, and revision surgery. Each of these procedures addresses a different anatomical issue.
The starting point for planning is identifying what is structurally changing. Is the concern primarily loss of volume? Excess weight? Skin laxity? Asymmetry? A clear understanding of the underlying issue shapes the surgical approach and helps determine whether surgery is appropriate at all.
Breast Augmentation
Breast augmentation is performed to increase volume and enhance projection. This can be achieved with implants or with autologous fat transfer.
Patients considering implant-based enlargement may want to understand the differences between techniques in our detailed guide to breast augmentation. Those exploring treatment options can also review the clinical overview of the breast augmentation procedure.
Implant Augmentation
Implants provide the most predictable and measurable increase in size. They allow control over projection, upper pole fullness, and overall contour with a high degree of precision. For patients with minimal existing breast tissue, implants are often the only realistic way to achieve a significant increase in volume.
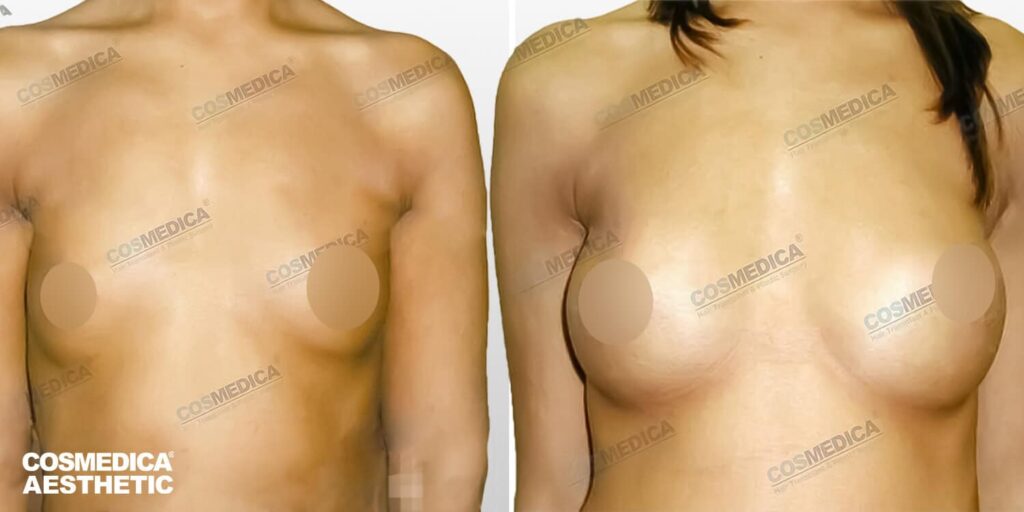
However, implants are medical devices rather than permanent biological tissue. They may require monitoring and, in some cases, replacement in the future. Long-term considerations form part of responsible planning, including awareness of potential complications such as capsular contracture, rupture, or displacement.
Surgical technique also plays a role in how implants look and feel. The incision location, implant placement relative to the chest muscle, and tissue thickness all influence final appearance.
Fat Transfer Augmentation
Fat transfer augmentation uses liposuction to harvest fat from areas such as the abdomen or thighs. The fat is processed and injected into the breast in small amounts to increase volume.
Because it uses the patient’s own tissue, fat transfer avoids placing a foreign device. Many patients prefer this aspect. The result often feels soft and can appear subtle and natural. However, the increase in size is typically modest compared to implants. Some of the transferred fat will be reabsorbed during healing, meaning the final result stabilises over several months.
Fat transfer also depends on having adequate donor fat. Very lean individuals may not be ideal candidates. It does not significantly tighten loose skin, so it may not correct sagging without a lift.
The choice between implants and fat transfer depends on anatomy, expectations, and tolerance for future maintenance.
Breast Lift (Mastopexy)
A breast lift reshapes and repositions the breast tissue to correct sagging, medically referred to as ptosis. Unlike augmentation, a lift does not primarily increase volume. Instead, it elevates the nipple position and removes excess skin to improve contour. Patients considering surgical correction of sagging can learn more about the breast lift procedure and how it is planned.
Sagging breasts develop gradually due to a combination of factors including ageing, pregnancy, breastfeeding, weight fluctuations, and genetic predisposition. Skin elasticity decreases over time, and supporting ligaments stretch. You can read more about breast lift after pregnancy and how tissue changes affect planning.
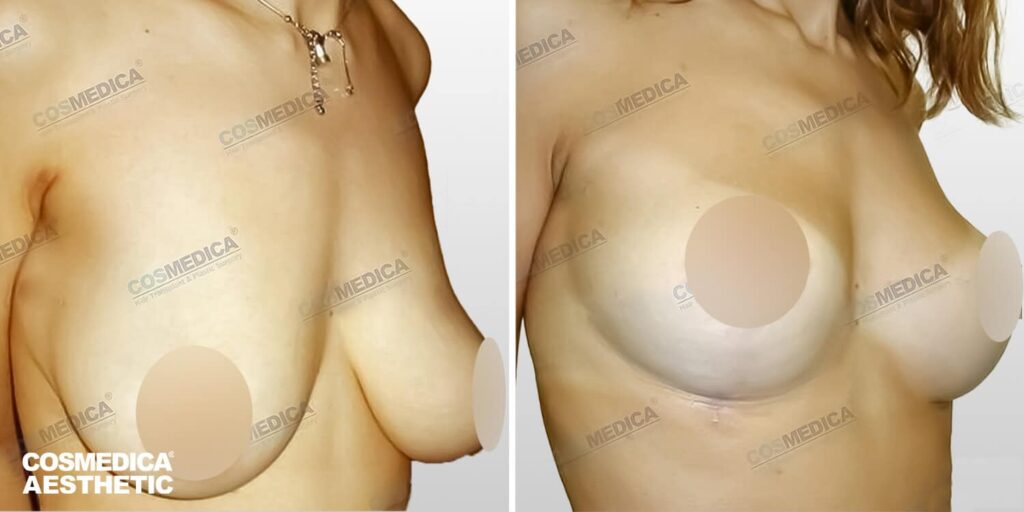
The degree of sagging determines the surgical technique and scar pattern. Mild cases may require limited incisions, while more advanced ptosis requires more extensive reshaping. While scars fade over time, they are permanent. Understanding scar placement and healing timelines is part of informed decision-making.
In cases where volume loss accompanies sagging, a lift may be combined with augmentation to restore both fullness and position.
Breast Reduction
Breast reduction decreases size and weight by removing excess glandular tissue, fat, and skin. While cosmetic improvement is part of the outcome, many patients seek reduction to relieve physical symptoms.
Large breasts can contribute to chronic neck pain, shoulder grooving from bra straps, rashes beneath the breast fold, and difficulty participating in exercise. Reduction can improve physical comfort as well as body proportion.
Recovery is gradual. Swelling and tightness are common in the early phase. Activity restrictions are usually advised during initial healing, with a gradual return to normal movement over several weeks. Final shape continues to settle as swelling resolves and scars mature.
Implant Characteristics and Surgical Planning
When implants are chosen, several design variables influence results. These include fill material, shape, projection, and surface texture.
Silicone implants contain cohesive gel and are often described as having a more natural feel. Saline implants are filled with sterile saltwater and visibly deflate if rupture occurs. Both types are widely used and regulated. The choice depends on anatomy, personal preference, and understanding of monitoring recommendations.
Implant shape also matters. Round implants tend to provide more fullness in the upper breast, while anatomical implants are shaped to mimic a natural slope. Projection refers to how far the implant extends forward from the chest wall. Selecting projection based purely on cup size can lead to disproportion; chest width, ribcage shape, and tissue thickness must all be considered.
Surface texture has received attention due to past associations between certain textured implants and a rare lymphoma known as BIA-ALCL. Current implant selection reflects updated safety guidance and regulatory oversight.
Implant Placement
Implants may be positioned above the chest muscle, below it, or using a dual-plane approach. Placement affects contour, early recovery discomfort, and how the implant behaves during movement.
Above-muscle placement may involve less initial tightness but requires sufficient natural tissue coverage. Below-muscle placement can soften upper contour in thinner patients but may feel tighter during early healing. Dual-plane techniques combine elements of both.
There is no universal best option. Placement decisions depend on tissue thickness, lifestyle, and aesthetic goals.
Revision Surgery and Implant Removal
Breast surgery does not always end with the first procedure. Revision surgery may be necessary due to complications, aesthetic dissatisfaction, implant rupture, or natural changes over time.
Capsular contracture, in which scar tissue around an implant tightens and distorts shape, is one recognised reason for revision. Some patients also choose implant removal without replacement.
Revision procedures are often more technically complex than primary surgery because scar tissue and altered anatomy must be considered carefully.
Recovery Timeline
Recovery varies depending on procedure type, individual health, and adherence to post-operative instructions.
In the early phase, swelling, bruising, and tightness are common. Sensation changes may occur temporarily. Activity restrictions are typically recommended during the first weeks, particularly avoiding heavy lifting and intense upper-body exercise.
Improvement occurs in stages rather than instantly. While many patients return to desk-based work within a couple of weeks, full healing continues for several months. Scars gradually mature and soften over time.
Risks and Complications
All surgery carries inherent risk. General risks of plastic surgery include infection, bleeding, delayed wound healing, and scarring concerns.
Implant-specific risks include rupture, displacement (double bubble breast), capsular contracture, and the possibility of future revision surgery. While serious complications are uncommon, understanding them supports informed consent and realistic expectations.
When Breast Surgery Is Not Recommended
Breast surgery is not appropriate for everyone. In some cases, postponing or avoiding surgery may be the safer decision.
Active infection, untreated medical conditions, uncontrolled diabetes, or significant cardiovascular disease can increase surgical risk. Smoking, particularly heavy smoking, impairs wound healing and may require cessation before proceeding.
Surgery may also be discouraged when expectations are unrealistic or when emotional distress is the primary motivation without clear anatomical concerns. Patients experiencing untreated body dysmorphic disorder or significant psychological instability may benefit from further assessment before considering surgery.
Pregnancy, ongoing breastfeeding, or unstable body weight can also influence timing. In such situations, waiting may lead to safer and more predictable outcomes.
A responsible surgical plan includes recognising when surgery should not proceed.
Long-Term Considerations
Breast surgery changes anatomy but does not stop natural ageing or biological processes. Pregnancy, weight fluctuations, and hormonal changes can alter breast appearance after surgery.
Breast implants are not lifetime devices. Some remain intact for many years, while others require earlier replacement. Monitoring recommendations vary based on implant type and evolving medical guidance.
Patients considering surgery should think beyond the first result and consider how their goals may evolve over time.
Choosing the Appropriate Procedure
Selecting the right breast surgery procedure requires aligning anatomy, goals, and long-term expectations. A thoughtful consultation process typically involves physical assessment, discussion of lifestyle factors, and exploration of alternative approaches.
Rather than focusing solely on size, it is more productive to focus on proportion, balance, and structural change. When expectations are realistic and planning is individualised, outcomes tend to be more stable and satisfactory.
Breast surgery encompasses more than augmentation alone. It includes reshaping, reduction for comfort, revision for complications, and long-term implant considerations. Understanding these distinctions builds a stronger foundation for decision-making and supports safer, more informed choices.